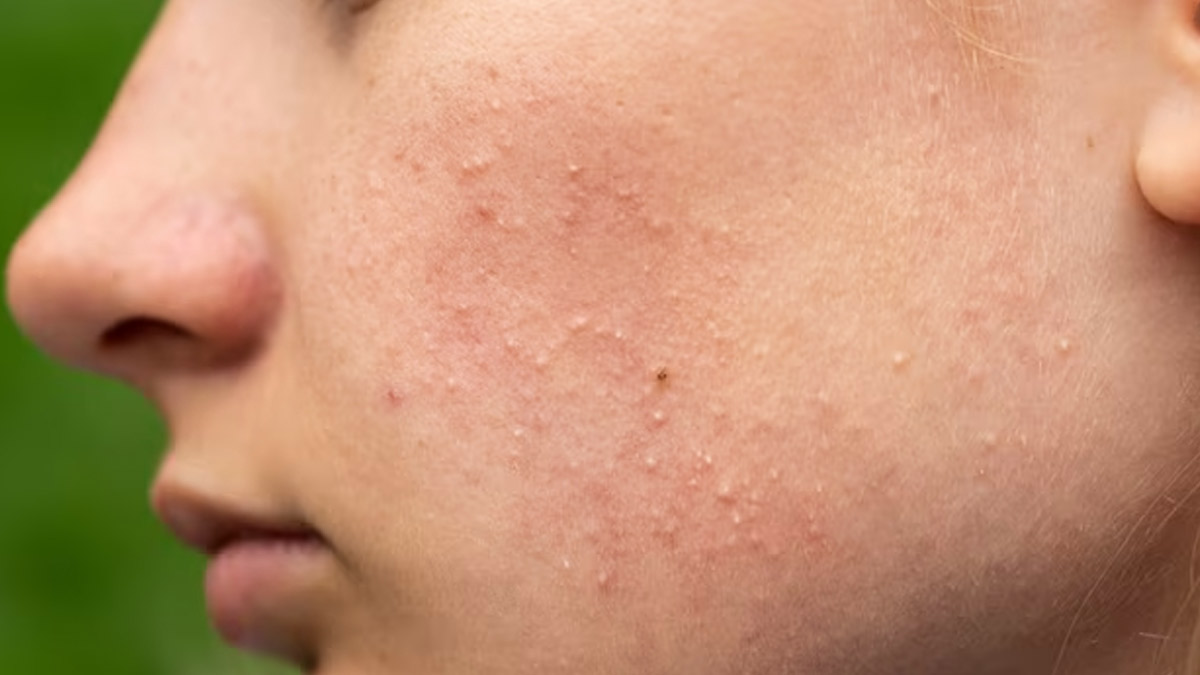
Milialar, those tiny white or yellowish bumps that sometimes appear on your skin, are a common but often misunderstood skin condition. While not a disease, these small cysts can be a cosmetic concern for many individuals. In this comprehensive blog, we’ll dive deep into what milia are, what causes them, the different types, and how you can effectively manage and prevent their occurrence. By the end, you’ll have a clear understanding of this skin condition and how to deal with it.
Milialar, often referred to as “milk spots,” are small, dome-shaped cysts that typically appear on the face. They are caused by the trapping of dead skin cells, oil, or keratin (a protein found in skin, hair, and nails) beneath the skin’s surface. Milialar can affect people of all ages, from infants to adults.
Deciphering Milialar
Milialar, with their distinct tiny, dome-shaped appearance, can easily be mistaken for whiteheads. However, they are far from being just another form of acne. Milia are small cysts filled with keratin, a protein found in our skin, hair, and nails. These cysts reside just beneath the skin’s surface, giving rise to the characteristic bumps.
While milialar can occur anywhere on the body, they most commonly make their appearance on the face, particularly around the eyes, nose, and cheeks. What’s intriguing about milia is that they are not exclusive to any particular age group; they can affect individuals of all ages.
Types of Milia
There are several types of milia, including primary, secondary, and milia en plaque. We’ll explore each type to give you a comprehensive understanding of this condition.
Primary Milia: Common in Infants
Primary milia are often seen in infants and tend to resolve on their own within a few weeks. In this section, we’ll explore the characteristics of primary milia, their typical duration, and how to manage and prevent them.
- Characteristics
Primary milia in infants have distinct characteristics. Understanding these features helps distinguish them from other skin conditions.
- Duration and Treatment
Learn how long primary milia typically lasts in infants and why they tend to disappear without the need for medical intervention.
Secondary Milia: From Skin Damage
Secondary milia can occur in response to skin damage or injury, such as burns, sunburn, or blistering. This section explores the causes of secondary milia and how to manage them effectively.
- Causes
Discover the various causes of secondary milia, including skin injuries and trauma.
- Managing Secondary Milia
Secondary milia can be more persistent. Learn how to deal with them and minimize their impact on your skin.
Milia en Plaque: A Rare Variant
Milia en plaque is a rare form that appears as multiple milia on an inflamed, raised patch of skin. We’ll delve into the unique characteristics and potential treatments for this variant.
- Appearance
Understand the distinct appearance of milia en plaque and how it differs from other types of milia.
What Causes Milialar?
Milialar can result from various factors, and understanding these causes is essential for effective management and prevention. We’ll delve into the key causes, including clogged pores, the use of certain skin products, and excessive sun exposure.
Clogged Pores: Clogged pores are a primary cause of milia. When dead skin cells and sebum (skin oil) become trapped, they can form milia. We’ll explore how these clogs occur and what you can do to prevent them.
Skin Products: Certain heavy or oil-based skin care products can contribute to milia formation. This section discusses the types of products to be cautious about and how to choose the right skincare items.
Sun Exposure: Excessive sun exposure and sun damage can lead to secondary milia. We’ll cover how UV radiation affects your skin and steps you can take to protect yourself from the sun’s harmful effects.
Keratin Entrapment: Milia originate from the entrapment of keratin, the skin protein, under the skin’s surface. This occurs when sweat ducts or hair follicles become clogged, preventing the natural shedding of skin cells.
Physical Skin Damage: Skin damage resulting from burns, blisters, abrasions, or other forms of trauma can lead to secondary milia. These bumps often appear during the healing process.
Certain Medications: The use of topical corticosteroids and specific medications may increase the risk of milia formation.
Genetics: Some individuals may have a genetic predisposition to developing milia.
Managing and Preventing Milia
Now that you have a thorough understanding of milia and their causes, let’s explore how to effectively manage and prevent them. This section covers several practical tips, including gentle exfoliation, the use of non-comedogenic products, sun protection, professional extraction, and why you should avoid squeezing milia at home.
Gentle Exfoliation: Regular, gentle exfoliation with a mild exfoliant can help remove dead skin cells, reducing the risk of milia.
Non-Comedogenic Products: Use non-comedogenic skin care products that are less likely to clog pores and contribute to milia formation.
Sun Protection: Protect your skin from excessive sun exposure by using sunscreen and wearing protective clothing.
Professional Extraction: For stubborn or persistent milia, consider consulting a dermatologist who can safely extract them.
Avoiding Squeezing: Refrain from attempting to squeeze or pop milia at home, as this can lead to skin irritation and scarring.
Professional Extraction: Dermatologists or licensed skincare professionals can safely extract milia using sterile instruments like needles or scalpels. Attempting this at home is discouraged, as it carries the risk of infection and scarring.
Topical Retinoids: Prescription retinoid creams can promote skin cell turnover and help clear milia over time.
Microdermabrasion: This non-invasive procedure gently exfoliates the skin’s surface, assisting in milia removal.
Chemical Peels: Chemical peels exfoliate the top skin layer, effectively addressing milia.
Cryotherapy: Cryotherapy involves freezing the milia with liquid nitrogen, causing them to fall off.
Hyfrecation: This medical procedure employs an electrical current to eliminate milia by drying them out.
Lancing: In this controlled procedure, a dermatologist makes a small incision in the milia and then manually extracts the contents.
Conclusion
In this extensive blog post, we’ve unveiled the mystery of “milk spots” by providing a comprehensive overview of milia, their types, causes, and effective management and prevention strategies.
Milia, while not a disease, can be an aesthetic concern for many people. Understanding what causes milia and how to manage and prevent them is essential for maintaining healthy skin. Remember that patience and proper skin care are key when dealing with milia. If you have persistent or bothersome milia, it’s advisable to seek the guidance of a dermatologist who can provide professional assistance.
By the end of this blog post, you’ll have gained a thorough understanding of milia and how to deal with this common skin condition. Whether you’re looking to manage existing milia or prevent their occurrence, you’ll be well-equipped with the knowledge to take care of your skin effectively.